Chimeric antigen receptors targeting Herpesvirus entry mediator
Introduction
- The immune system has certain mechanisms to protect the body from various diseases, especially the detection and elimination of pathogens such as germs and viruses. Also, the immune system distinguishes healthy cells from diseased cells to prevent the formation and growth of cancer, which is done by recognizing antigens that represent the transition from healthy to morbid. As an immunotherapy treatment to cancer, researches on cell therapy are being actively conducted to strengthen or genetically alter immune cells.
- In the past, immunotherapy used an ex vivo proliferative method using T cells separated from tumors, but it was difficult to control the proliferation of T cells and acquire antigen-specific T cells because of the formation of heterogeneous T cell groups. Thus, studies have been actively conducted to apply to immunotherapy the artificial receptor (chimeric antigen receptor) based on gene recombination technology. CAR is an artificial receptor designed for T cells to recognize specific antigen and represent cell toxicity, consisting of an extracellular binding domain, a membrane domain, and an intracellular signal domain that recognizes cancer cells as an antigen. The extracellular binding domain recognizes the membrane ligand of cancer cells with certain antigens, the transmembrane area connects the extracellular junction area with the intracellular signal area, and the intracellular signal area sends signals from the extracellular junction area to activate the T cell immune response.
- Immunotherapy using CAR-T cells has a therapeutic effect on cancer in clinical trials. In clinical trials of five Acute Lymphoblastic Leukemia patients with high mortality and poor efficacy in chemotherapy, the treatment effect was shown at a rapid pace, and the study of 44 acute lymphocytic leukemia patients showed an increasement in the overall survival period after CAR-T cell treatment. Also, CD19 CAR-T cells showed better therapeutic effect than conventional treatment Cyclophosphamide alone or Fludarabine's combination therapy in B cell non-Hodgkin's lymphoma or Chronic Leukemia patients.
- CAR-T cells that may be attractive to immune agents, especially cancer treatments, contain potential risk factors that may cause side effects to normal cells or tissues, resulting from the recognition of antigens in normal tissues. As a mean to overcome this, next-generation CAR-T cells have increased the ability to recognize cancer cells-specific antigen by adding artificial receptors that being developed. But on the other hand, it is also important to find new cancer-specific markers with few side effects such as the above.
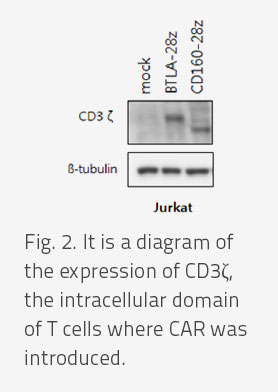
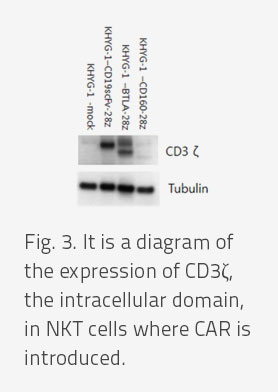
- To excavate new cancer-specific markers, CAR-T was developed for HVEM, which is commonly expressed in Melanoma. Unlike normal CAR-T made using the scFv of antibodies, this study uses the BTLA or CD160 protein itself, which binds with HVEM as a ligand, instead of the activation of CAR-T by binding between antibodies and target proteins, the CAR-T active induction by coupling with HVEM and its ligand is a new study result.